A Comprehensive Guide to Psoriasis:
Understanding, Managing, and Treating This Skin Disease
Description
Within the confines of this comprehensive guide, you will find nuanced insights on psoriasis, a common but often misunderstood skin disease. The information encapsulates everything from what to do and what not to do, recent medication breakthroughs, as well as potential linkages to auto immune health disorders.
Introduction
One's journey with psoriasis might be fraught
with annoying symptoms and social difficulties, but with proper knowledge,
support, and treatments, living a full life is entirely feasible.
What is Psoriasis?
Contrary to popular belief, psoriasis is not
simply a ‘skin disease’. It is an auto immune health disorder that primarily
manifests as skin inflammation and scaling, scientifically termed as 'plaques'.
Understanding Psoriasis
While this disorder may primarily present
visible skin symptoms, it is crucial to understand that it originates within
the immune system. Misdirected immune response aggravates skin cells'
production, leading to the telltale plaques associated with the disease.
The Psoriasis Spectrum
The severity and manifestation of psoriasis
can greatly differ from individual to individual. Some people may merely
experience minor localized scaling while others might be plagued by psoriatic
eruptions encompassing the entire body.
Types of Psoriasis
Knowing the type of psoriasis you have plays a
significant role in your management and treatment plan. Some common types
include plaque psoriasis, inverse psoriasis, guttate psoriasis, pustular
psoriasis, and erythrodermic psoriasis.
Symptoms of Psoriasis
The most common symptoms include red patches
of skin covered with thick, silvery scales, dry and cracked skin that may
bleed, and itching, burning, or soreness. The nails and joints may also get
affected resulting in pitted nails or psoriatic arthritis, respectively.
What Triggers Psoriasis?
Triggers could encompass a wide range of
elements like stress, infections, certain medications, nicotine, and even
weather changes. Identifying and avoiding personal triggers are integral to
effective psoriasis management.
How to deal with Psoriasis
Misconceptions About
Psoriasis
It's important to debunk the lie that
psoriasis is contagious. It's rooted in an immune system malfunction and cannot
be 'caught' from affected individuals.
The Emotional Burden
Aside from the physical ailments, psoriasis
often brings a heavy emotional weight, dealing with the stares, misconceptions,
and its annoying omnipresence in everyday life. Offering emotional support or
seeking mental health professionals is highly recommended.
Psoriasis and Auto-Immune Disorders
Psoriasis may not confine its influence to the
skin. There is a known correlation between this condition and the onset of
other auto-immune disorders like Crohn’s disease.
Diagnosing Psoriasis
Generally, dermatologists can diagnose
psoriasis by examining the skin. However, if the diagnosis is doubtful, a
biopsy may be performed.
The Psoriasis Treatment Landscape
Treatment typically involves managing
symptoms, preventing flares, and slowing cell turnover. For many, a combination
of treatments - topical, phototherapy, and systemic medications - is effective.
New Medication Developments
Research into psoriasis treatment is
burgeoning. Besides the standard corticosteroids or light therapy, new
strategies such as biologics, which specifically target the immune response
triggering psoriasis, are offering patients new hope.
Lifestyle Changes for Managing Psoriasis
Healthy living is an astoundingly effective
form of management for psoriasis. Incorporating a nutrient-dense diet,
exercise, limiting alcohol consumption, and quitting smoking could
significantly reduce flare-ups.
When to Seek Medical Attention?
Psoriasis is a chronic disease that calls for
regular medical follow-ups. However, in case of severe, persistent flare-ups
and psychological distress, immediate medical attention is crucial.
Conclusion
Psoriasis is often a lifelong journey of
managing symptoms, navigating personal triggers, and medicating appropriately.
While it may be an arduous path, remember, with the right knowledge and
support, you are more than equipped to live a fulfilling life.
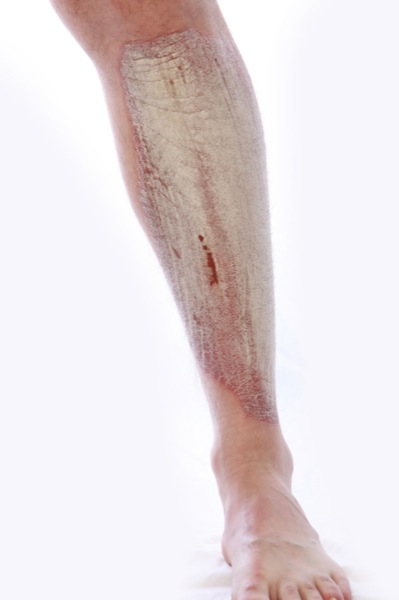 Psoriasis en la pierna
Psoriasis en la piernaPágina de inicio
Mapa del sitio
Mapa del sitio en orden alfabético